Fillings (Decay Or Broken Teeth)
Fillings (Decay Or Broken Teeth)
Fillings (Decay Or Broken Teeth)
When decay is relatively small, treatment involves removal of only what is necessary. Modern materials allow as much tooth to be preserved as possible. Modern techniques include ‘key-hole’-like surgery for preparing the decayed dentine whilst leaving much of the supportive and strong outer enamel intact. Of course, for extremely weakened areas of the tooth, more extensive restorations may be indicated.
Fillings do involve the dentine, a living part of the tooth. Dentine can detect hot, cold, sweet and touch- but only translate all those different things as pain. Obviously, this is one sensation that we don’t aim for you to encounter at Cornerstone Dental. Our dentists use a specially compounded numbing gel before administering the anaesthetic. This makes for virtually painless injections. In conjunction with atraumatic anaesthetic techniques, a fear of needles need be something of the past.

A Dental Filling: Step-by-step
These pictures are a case example of a cosmetic tooth-coloured filling done here at Cornerstone Dental.
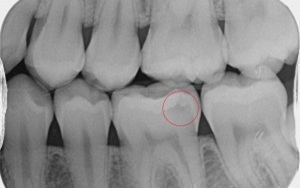
Step 1
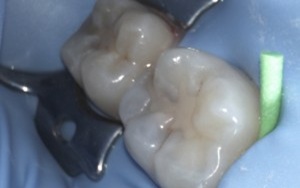
Step 2
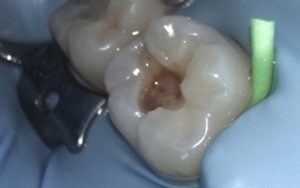
Step 3
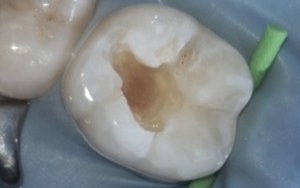
Step 4
Soft decay is removed and the tooth etched.
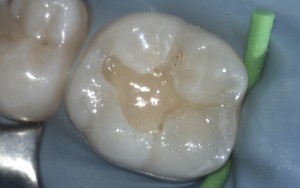
Step 5
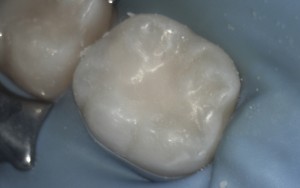
Step 6
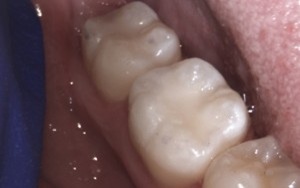
Step 7
Types of Fillings
Minimally invasive fillings are placed on the basis that an appropriate amount of decayed tooth is removed. The tooth is repaired with a tooth-coloured restoration that bonds to and supports the remaining tooth structure. There are several different types of ‘white’ fillings.
Prior to selecting which one (or sometimes a combination), the dentist will consider the following factors:
- How the material will bond to the tooth
- How the material will seal the cavity and prevent new decay from occurring
- If the material can remineralise the surrounding tooth
- How does the material wear; its strength
- Will the material protects the surrounding tooth from fracture
- Aesthetics
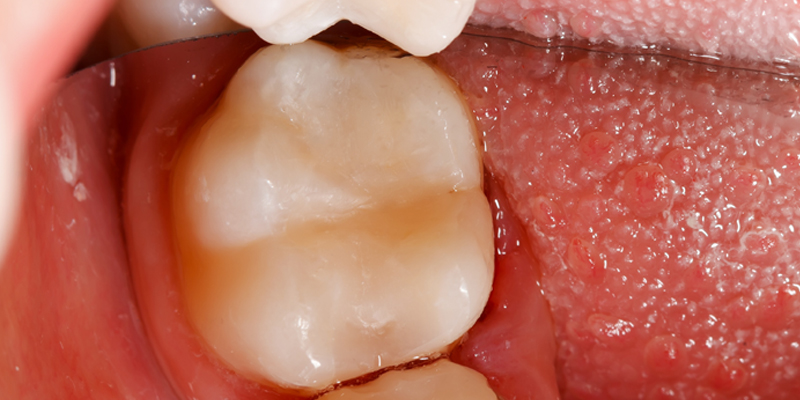
Glass Ionomer Cement
Glass ionomer is a water-based cement. It is formed from the reaction of an acid (polyalkenoic acid) with a powdered glass base (including fluoride, calcium or strontium aluminosilicate). When the dentist is ready to use this material, the tooth is first conditioned, and an assistant will mix a capsule containing the filling’s components into a tooth-coloured putty.
‘Fuji VII’, ‘Riva Protect’
This is a high fluoride releasing filling material that allows enhanced remineralisation of surrounding tooth structure. It is more of a solid white colour, so it useful as a base under deep fillings, fissure sealants, and temporary fillings to stabilize decay when many teeth are involved. It may also prevent plaque from growing around the filling itself. A pink-coloured form of this filling has added pigments that makes it heat up and set faster under blue light.
Glass ionomer is one of the best materials for a tooth with minor first-time decay on the biting surfaces.
Composite Resin
Composite Resins are ceramic-filled polymers which are set hard by blue light. The qualities of composite resin include excellent aesthetics, good physical properties like hardness. The major components inlcude a resin matrix (Bis-GMA), glass filler particles (containing aluminum, barium, strontium, zinc, zirconium or quartz), coupling agents and light activating agents. When set under blue light, composites can shrink slightly, so care must be taken to cure the filling in layers.
Composite adheres to the tooth by microscopically interlocking into the rough and jagged surface of cut, etched enamel. It does not bond as well to dentine, the living inner layer of the tooth, because it is always slightly moist, and resin is hydrophobic (similar to oil, doesn’t like water). We overcome this problem by placing glass ionomer as a base, and add the hard composite layer on top. This way the filling has the best of both worlds- the base layer releases fluoride and minerals, bonds to dentine and stops bacteria from growing. The top layer is hard and strong, bonds well to enamel, and has greater aesthetics.

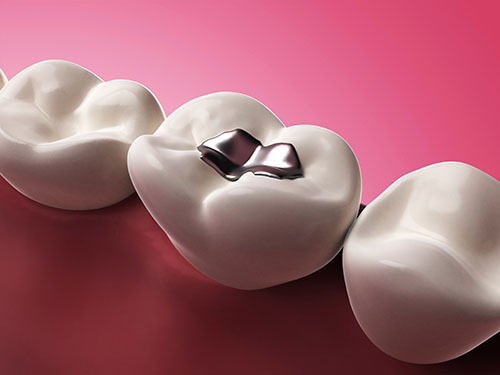
Amalgam
Taking into the account of the principles of minimal intervention, modern restorative practice, general public health and environmental principles, we limit the use of amalgam fillings in our treatment planning. However, we do not object to the use of amalgam fillings on the rare occasion where it may be the most appropriate restorative option, for example, for very large fillings when a crown is not financially viable, and where is difficult keep an area dry enough.
Unfortunately, many patients have been advised or request to have existing amalgam fillings replaced in the mistaken belief that this will improve their general health, or result in a cure for chronic afflictions. Health authorities consistently reject these reasons for removal, or avoidance for placement, citing evidence from many very large, significant studies.
